AI insurance claims processing is the application of machine learning, natural language processing, and computer vision to automate the intake, classification, extraction, adjudication, and settlement of insurance claims. Unlike point-solution automation, document AI operates across the full claims lifecycle, transforming unstructured PDFs, images, and forms into structured, auditable data that drives faster decisions with fewer human touchpoints.
Why Manual Claims Handling Is Now a Competitive Liability
AI insurance claims processing has crossed the threshold from exploratory investment to operational necessity. McKinsey (2024) estimates that a full end-to-end claims domain transformation yields up to 14 times the impact of isolated point solutions, yet BCG’s 2024 Build for the Future study found that only 7% of insurance carriers have successfully scaled AI beyond pilot programmes. The gap between potential and reality is not a technology problem. It is a commitment problem.
The customer pressure is real. Accenture (2022) found that 31% of policyholders who filed recent claims were dissatisfied, with 60% citing settlement speed as the primary cause. Adjusters managing 150 to 200 open claims simultaneously cannot close that gap manually. The bottleneck is not effort, it is information. Documents arrive in every format imaginable: scanned PDFs, mobile photos, handwritten forms, medical discharge summaries, repair invoices, and police reports. Processing them manually creates delays measured in days. AI processes them in seconds.
The urgency is especially pronounced in Asia-Pacific. Market data (2025) shows the APAC AI insurance market reached USD 2.80 billion in 2025 and is growing at 42.2%, the fastest regional growth rate globally. Carriers in India, China, Singapore, and Southeast Asia are not playing catch-up. Many are leapfrogging directly to generative and agentic AI on cloud-native stacks, unburdened by legacy mainframes.
“The insurers winning with AI are not automating tasks, they are rewiring entire claims domains.”
How Document AI Works Across the Claims Lifecycle
Document AI in insurance applies OCR, natural language processing, and vision-language models to extract structured fields from unstructured documents at every stage of the claims lifecycle, from first notice of loss through settlement. Each stage produces structured data that feeds the next, creating a chain of decisions that can be automated, audited, and continuously improved.
Stage 1: First Notice of Loss (FNOL) Intake
The claim begins when a policyholder submits a loss event. AI-powered intake channels, including mobile apps, voice agents, and web portals, capture the initial report and extract key fields: incident date, location, policy number, and loss description. AWS’s open-source serverless EDA reference implementation demonstrates this pattern, using EventBridge to route submission events from a React frontend through document validation and into downstream processing queues in real time.
Stage 2: Document Classification and Field Extraction
Once documents arrive, a multi-stage extraction pipeline classifies each document type before attempting field extraction. A 2025 arXiv paper by researchers working on real-world claim pipelines (arXiv:2601.01897) describes a hybrid architecture that uses compact Vision-Language Models with multilingual OCR, decomposing the task into pre-processing, hybrid classification, adaptive extraction, and post-processing. This matters because heterogeneous document sets, spanning different templates, languages, and layouts, defeat rule-based approaches. Layout-aware transformers such as LayoutLM and DocLLM handle variable formats far better than template-matching logic.
Stage 3: Cross-Reference Validation and Fraud Screening
Extracted fields are validated against policy data and run through fraud signal models. Accenture’s agentic AI framework (2026) describes two agent classes at this stage: Super Agents that handle intake, summarisation, verification, and adjudication; and Utility Agents that extract and validate document data while monitoring performance. This separation of concerns keeps the architecture modular and auditable, a requirement regulators across APAC and Europe increasingly enforce.
Stage 4: Adjudication and Settlement
Validated claims pass to a rules engine. Routine claims are auto-adjudicated through straight-through processing. Complex or flagged claims escalate to human reviewers with AI-generated summaries and recommended decisions. Accenture’s implementation benchmarks show a 74% reduction in claims settlement time and 80% accuracy on automated health claim processing, with the remaining 20% correctly escalated for human correction.
“Document AI does not replace adjusters, it removes the 80% of their day spent finding information.”
Architecture of an AI-Driven Claims Processing System
A modern AI claims architecture layers five processing tiers connected by an event-driven messaging backbone. Each layer is independently scalable and replaceable, a design principle that avoids the vendor lock-in that stalls enterprise AI programmes.
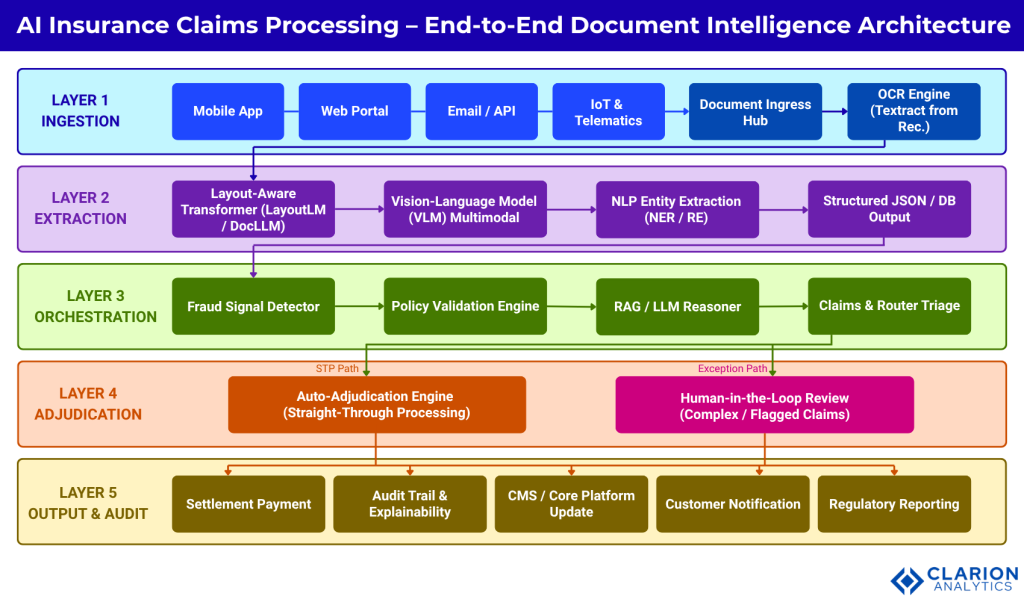
Figure 1 caption: The diagram shows five processing layers. Layer 1 captures multi-channel document submissions via OCR engines such as AWS Textract and Azure Form Recognizer. Layer 2 applies layout-aware transformers and VLMs to extract structured JSON from any document type. Layer 3 orchestrates fraud signal detection, policy validation, and RAG-based LLM reasoning. Layer 4 routes claims to auto-adjudication or human-in-the-loop review for complex cases. Layer 5 delivers settlement payments, audit trails, CMS updates, customer notifications, and regulatory reporting.
Code Snippet 1: Event-Driven Claim Routing
Source: aws-samples/serverless-eda-insurance-claims-processing
yaml
# EventBridge rule: routes claim events by type
# to downstream Lambda processors
EventPattern:
source:
- insurance.claims
detail-type:
- ClaimSubmitted
detail:
claimType:
- AUTO
- PROPERTY
- HEALTH
Targets:
- DocumentExtractionFunction
- FraudSignalFunction
- PolicyValidationFunctionThis pattern shows how document AI extraction output becomes an event that triggers parallel downstream processing. Instead of a sequential waterfall, fraud screening, policy validation, and extraction run concurrently, cutting end-to-end latency. Every event is logged to an audit stream, satisfying regulatory traceability requirements without additional instrumentation.
The Technology Stack: What Leading Insurers Are Actually Using
Selecting the right combination of tools depends on the document types in scope, the volume of claims, the degree of multilingual content, and the regulatory environment. NLP survey research (Ly, Uthayasooriyar and Wang, SCOR, 2020) shows that no single technique dominates across all claim types. The answer is always a layered stack.
| Approach | Key Strength | Best Used When |
|---|---|---|
| Rule-Based RPA | Deterministic, auditable, fast to deploy | Document types are highly structured and consistent (e.g. standard claim forms) |
| NLP + Layout-Aware Transformers (LayoutLM, DocLLM) | Handles variable document layouts; extracts fields regardless of template | Processing heterogeneous docs: medical records, repair invoices, discharge summaries |
| Vision-Language Models (VLMs) + Multimodal AI | Processes scanned images, handwritten forms, photos of damage | Documents arrive as images or photos; multilingual environments common |
| RAG + LLM Orchestration (LlamaIndex, LangChain) | Contextual reasoning against policy documents; natural language Q&A | Adjudication support, coverage determination, policy cross-referencing |
| Agentic AI (Multi-Agent Systems) | End-to-end automation of complex, multi-step claims with judgment | High-volume, multi-document claims requiring fraud, medical, and legal orchestration |
Code Snippet 2: Document Extraction Pipeline
Source: MSUSAzureAccelerators/AI-Powered-Insurance-Claims-Automation-Accelerator
yaml
# Logic App trigger: new document in Blob Storage
trigger: When_a_blob_is_added_or_modified
container: claims-inbox
# Action 1: Call Azure Form Recognizer
action: Analyze_document
model: prebuilt-document
input: triggerBody()?['Path']
# Action 2: Parse extracted fields
action: Parse_JSON
schema: ClaimDocument
content: body('Analyze_document')
# Action 3: Write structured record to Cosmos DB
action: Create_or_update_document
collection: claims-structured
body: parsedFields + metadataThis pipeline illustrates the handoff between document AI and the claims management system. The Logic App monitors a Blob container for incoming documents, triggers Form Recognizer to extract structured fields, and writes the resulting JSON to Cosmos DB for downstream adjudication. The same pattern works with any document AI engine, as the orchestration fabric is provider-agnostic.
“The gap between the 7% of insurers who have scaled AI and the 93% still in pilot purgatory is not technology, it is domain commitment.”
Claims Automation in APAC: A Region Moving Faster Than You Think
Asia-Pacific is the fastest-growing region for AI claims automation, with the automated claims management market expanding at 18.7% CAGR through 2030, and the broader AI in insurance market growing even faster. This is not a future trend. It is happening now.
Several structural factors accelerate APAC adoption. Many carriers in India, Indonesia, and Southeast Asia launched their digital platforms within the last decade, meaning they carry no legacy mainframe debt. They deploy generative and agentic AI directly on cloud-native stacks. Government-led digital transformation initiatives in India, China, and Singapore provide infrastructure and regulatory tailwind. Digital insurance sales in India grew over 40% annually between 2020 and 2024, according to the Indian Institute of Management Ahmedabad. Over 150 insurtech firms were operating across the region as of 2024, creating an ecosystem of specialised vendors building for local languages, document formats, and regulatory environments.
Incumbent carriers are responding. Tokio Marine and Sompo Japan have deployed AI-driven platforms for risk assessment and claims automation. MetLife partnered with Sprout.ai in July 2025 to accelerate AI claims processing across US, Asian, and Latin American markets. The APAC leapfrog story is real, and it is compressing the timeline for carriers in every other region.
Implementation Roadmap: From Pilot to Production at Scale
Teams building this at scale typically find the same three failure modes. First, they start with a use case instead of a domain, automating email acknowledgement but leaving extraction and adjudication layers manual. Second, they underinvest in data quality, discovering too late that the model is only as good as the ground truth it was trained on. Third, they defer the governance conversation, producing a system that cannot explain its decisions to regulators or to claimants.
In practice, the fastest path from pilot to production follows three phases.
Phase 1 is domain mapping: identify the top five document types by volume and error rate, and quantify the time adjusters currently spend locating information within each. This becomes your ROI baseline and your prioritisation matrix.
Phase 2 is modular integration: deploy the extraction layer first, connecting document AI output to your existing claims management system via an event-driven API rather than a full re-architecture. This approach, advocated in Accenture’s agentic AI framework, means carriers can enhance claims decisions through summarisation and synthesis without a radical change of tech stack.
Phase 3 is governance-first scaling: build the audit trail and explainability layer from day one, not as an afterthought. Every auto-adjudication decision should log the documents reviewed, the fields extracted, the rules applied, and the confidence score.
The payoff for disciplined execution is substantial. McKinsey’s 2025 analysis of Aviva, which deployed over 80 AI models in its claims domain, shows a 23-day reduction in complex liability assessment time, a 65% reduction in customer complaints, and savings exceeding £60 million in a single year. That result was not delivered by a chatbot or a point solution. It was delivered by rewiring the entire claims domain.
“Every insurer has a claims AI pilot. The question is whether it has a claims AI operating model.”
Frequently Asked Questions
How does AI insurance claims processing work step by step?
A claimant submits documents via mobile, portal, or email. An OCR engine digitises the content. NLP and vision-language models extract structured fields. A rules engine cross-checks policy data and runs fraud screens. Routine claims are auto-adjudicated; complex cases escalate to human reviewers. The entire cycle can complete in minutes rather than days, with every decision logged for audit.
What documents can AI extract data from in a claims workflow?
AI document processing handles PDFs, scanned images, photos of damage, medical discharge summaries, repair invoices, police reports, and handwritten forms. Layout-aware transformer models such as LayoutLM and multimodal vision-language models handle variable templates and multilingual content, making them suitable for the heterogeneous document sets common in health, auto, and property claims.
How accurate is AI in insurance document processing?
Production systems report 80% accuracy for automated health claim processing, with the remaining 20% escalated to human reviewers. Accenture benchmarks show AI classification is 30% more accurate than manual processing. Accuracy improves continuously as models are retrained on confirmed claim outcomes stored in the system of record.
What is the ROI of automating claims with document AI?
Aviva’s 2024 AI claims transformation saved £60 million in one year and cut liability assessment time by 23 days. Accenture deployments show a 74% reduction in settlement time. BCG research shows focused AI in complex P&C lines delivers up to 36% efficiency gains, with full domain transformation producing up to 14 times the impact of point solutions.
How is claims automation different in APAC compared to other regions?
APAC carriers benefit from lighter legacy debt, mobile-first customer behaviour, and government-backed digital infrastructure. Asia-Pacific AI claims automation is growing at 18.7% CAGR, the fastest globally. Many APAC insurtechs bypass traditional RPA entirely, deploying generative and agentic AI directly on cloud-native stacks, reaching production scale faster than counterparts in more legacy-heavy markets.
Conclusion: Three Decisions That Separate Leaders from Laggards
Three insights from this analysis deserve to be carried forward into any transformation roadmap.
First, domain commitment produces exponential returns. McKinsey’s analysis is clear: end-to-end claims domain transformation yields up to 14 times the impact of isolated use cases. Piloting AI for email acknowledgement while leaving extraction and adjudication manual produces only marginal gains.
Second, document AI is the connective tissue of the claims lifecycle, not just an intake tool. Every stage from FNOL through settlement depends on the quality of field extraction. Getting the extraction layer right makes every downstream system smarter.
Third, APAC carriers have a structural advantage they are already exercising. Cloud-native infrastructure, government digital mandates, and a new generation of local insurtechs are compressing the adoption timeline. The window for incumbents in every region to close the gap is narrowing.
The technology is proven. The architecture is documented. The ROI is quantified. The remaining question is the one that separates transformers from experimenters: Is your claims transformation roadmap built around use cases, or around the domain?